PRIMROSE CLINCIAL TRIAL FOR RADIATION DERMATITIS IN BREAST CANCER PATIENTS
Radiation dermatitis experienced by many patients receiving radiation therapy (RT) for cancer and is most common in patients with cancers of the breast, head and neck, and prostate1. Oxidative stress produced by RT results in dose-dependent skin damage, which can manifest as radiation dermatitis. RT typically destroys cellular structures in exposed skin leading to ulceration, necrosis, and fibrosis of skin tissue. In addition to its direct physical complications, such as severe pain, long-term scarring, and fibrosis, as well as the resulting impact on overall quality of life, radiation dermatitis can also be a dose-limiting toxicity requiring changes to or cessation of the prescribed course of radiation therapy.
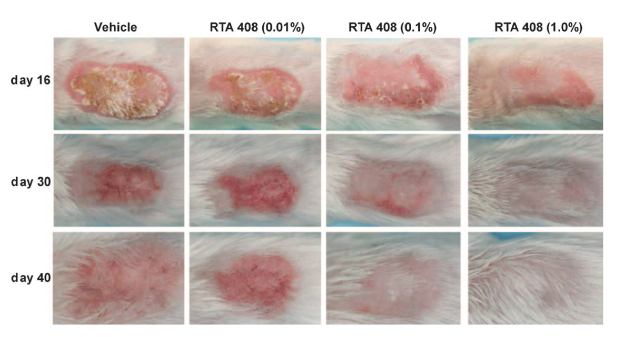
Currently, there are no approved agents for the prevention of radiation-induced dermatitis.The profound ability to protect tissues from ionizing radiation was one of the first and most consistent observations that were made with the AIM class of compounds. These protective effects result from the potent activation of Nrf2, which upregulates a battery of cytoprotective genes that directly protect cells from ROS and oxidative stress. Reata has completed a series of studies showing that RTA 408 is highly effective at mitigating the negative effects of radiation exposure, and is very potent in rodent models of radiation-induced dermatitis when applied topically. RTA 408 and other AIM analogs consistently outperform all other agents tested in these models of radiation-induced injury.
If you are interested in receiving regular updates on the progress of the PRIMROSE trial, please complete the contact form below:
[one_half]
New Study Tests Lotion To Treat Radiation Dermatitis in Breast Cancer Patients
 Irving, Texas based Reata Pharmaceuticals has announced enrollment of its first patient in a Phase 2 dose-ranging study examining the safety, tolerability, and efficacy of the company’s RTA 408 Lotion (3% and 0.5%) versus vehicle for prevention and treatment of radiation dermatitis in breast cancer patients for whom radiation therapy (RT) is recommended.
Irving, Texas based Reata Pharmaceuticals has announced enrollment of its first patient in a Phase 2 dose-ranging study examining the safety, tolerability, and efficacy of the company’s RTA 408 Lotion (3% and 0.5%) versus vehicle for prevention and treatment of radiation dermatitis in breast cancer patients for whom radiation therapy (RT) is recommended.
[/one_half]
[one_half_last]
[/one_half_last]
Clinical Trial Protocol
Radiation dermatitis is experienced by almost all patients (up to 95%) receiving radiation therapy for cancer. Radiation dermatitis can be a serious condition because, in addition to its direct physical complications and the resulting impact on overall quality of life, it can also be a dose-limiting toxicity requiring changes to the prescribed course of radiation therapy. The most common strategy employed in an attempt to prevent or minimize radiation dermatitis involves moisturization of the irradiated area, use of a mild soap to keep the area clean, and minimizing exposure to potential mechanical irritants, such as scratching and rough clothing. However, this strategy has been shown to lack clinically significant efficacy. Consequently, there is a clinical need for new treatments that are effective in protecting against radiotherapy-induced oxidative stress and the subsequent development of radiation dermatitis.
Based on data from previous studies in animals and humans, Reata believes that RTA 408 Lotion may effectively prevent and mitigate radiation dermatitis in oncology patients undergoing radiation therapy.
This randomized, double-blind, vehicle-controlled, parallel-group trial will study the efficacy, tolerability and safety of two concentrations of RTA 408 Lotion (3% and 0.5%) versus vehicle in patients with breast cancer for whom radiationtherapy is recommended.
- Grading of skin changes following radiation therapy [ Time Frame: 9 weeks (maximum of 13 weeks) ] [ Designated as safety issue: No ]
Grading of skin changes (using CTCAE grading scale) due to treatment with radiation therapy, following topical application of RTA 408 lotion or lotion vehicle
- Count of patients who experience a maximum radiation dermatitis grade of less than 2 [ Time Frame: 9 weeks (maximum of 13 weeks) ] [ Designated as safety issue: No ]
Count the number of patients who experience a maximum radiation dermatitis grade of less than 2 (based on CTCAE grading scale) due to treatment with radiation therapy, following topical application of RTA 408 lotion or lotion vehicle
- Adult female patients (18 to 75 years of age, inclusive);
- Patients diagnosed with ductal carcinoma in situ or non-inflammatory breast adenocarcinoma who have been referred for post-operative radiotherapy and have had no prior radiation treatment to that breast;
- Patients planning to undergo 3D conformal radiation therapy to the whole breast (as part of breast-conservation therapy / lumpectomy) or chest wall (as part of post-mastectomy irradiation), with or without treatment of regional lymph nodes (i.e., axillary, supraclavicular, or internal mammary), using one of the following treatment schedules:
- 45 – 50.4 Gy in 1.8 Gy per day, in addition to 10-16 Gy boost
- 46 – 50 Gy in 2 Gy per day, in addition to 10-16 Gy boost;
- Patients who received breast-conservation therapy / lumpectomy must be receiving ≥ 107% of the total radiation dose (calculated from the total radiation dose including boost) to any portion of the breast, based on radiation inhomogeneity, and/or have a breast volume ≥ 1200 cc;
- Patients may also be receiving sequential, neoadjuvant or adjuvant, chemotherapy;
Exclusion Criteria:
- Patients with Stage T4 breast cancer;
- Patients with prior radiation therapy;
- Patients with type V or VI skin according to the Fitzpatrick scale;
- Patients with bilateral breast cancer;
- Patients receiving partial breast irradiation therapy;
- Patients with uncontrolled diabetes (HbA1c > 11.0%, historical values within 6 months of screening are acceptable);
- Patients with collagen vascular disease or vasculitis;
- Patients with concurrent active malignancy other than adequately treated basal cell carcinoma of the skin or carcinoma in situ of the cervix;
- Patients with active bacterial, fungal or viral skin infections;
- Patients with known active hepatitis B or hepatitis C infection;
- Patients who intend to use any other topical cream, lotion or preparation applied to the radiation treatment area;
