 A new study recently highlighted a novel approach to radiation therapy for breast cancer patients receiving lumpectomies that may significantly cut down on their exposure to radiation and time spent in the hospital, requiring only a single dose at the same time of the surgery.
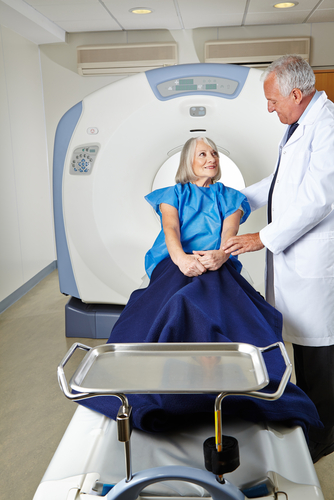
A new study recently highlighted a novel approach to radiation therapy for breast cancer patients receiving lumpectomies that may significantly cut down on their exposure to radiation and time spent in the hospital, requiring only a single dose at the same time of the surgery.
The new technique, which was recently highlighted in an article on Science Daily, was developed by researchers at Rush University Medical Center, who sought to improve the efficacy of radiation treatment by targeting it at the exact location of the lumpectomy. According to the article, the new technique, known as intraoperative radiation therapy (IORT), applies radiation therapy directly into the surgical site, just after a cancerous tumor has been removed: “a catheter-like device with a balloon at the tip is inserted into the lumpectomy cavity. The balloon is inflated with saline and the radiation therapy source docks precisely into the catheter to deliver radiation to the breast tissue surrounding the cavity where the tumor was removed, while avoiding radiation to nearby organs. At the end of radiation treatment, the balloon is deflated and easily removed and the cavity is closed.”
The IORT approach to delivering radiation therapy is markedly different from standard radiation treatment, which typically involves receiving one or two treatments daily for up to 6 weeks after a lumpectomy. The new technique is believed to be potentially more effective, since the radiation is delivered to the site of where cancer had been present — applied directly, as opposed to having to pass through the body. It also subjects breast cancer patients to far less radiation, which can lead to painful side effects, such as radiation dermatitis.
Dr. Katherine Kopkash, an assistant professor of surgery at Rush University Medical Center, explained how IORT gets breast cancer patients home from the hospital faster while appearing to offer comparable results to standard radiation approaches. “While recovery time from surgery with intraoperative radiation therapy is the same as surgeries performed without IORT,” she said, “the patients’ overall time spent in the hospital receiving treatments for breast cancer is drastically decreased. This option allows patients to return to their lives faster by potentially reducing the need for further therapies and enhancing their quality of life.” Dr. Kopkash sees the technique as particularly helpful for rural-based breast cancer patients who may live far away from hospitals and cannot readily commute daily for radiation treatment after surgery.
While relatively new to the U.S., IORT is not an altogether new radiation therapy approach, in that it has been performed in Europe since the 1990s. At present, the technique is mainly being used in early-stage breast cancer patients and those who are undergoing nipple-preserving mastectomy surgery. However, the prospect of the technique expanding to other scenarios in the future is certainly possible.
[adrotate group=”1″]